Vaccine Hesitancy: The Next Challenge in the Fight against COVID-19
Galilee Medical Center (Dror, Eisenbach, Mizrachi, Zigron, Srouji, Sela); Bar-Ilan University (Dror, Eisenbach, Mizrachi, Zigron, Srouji, Sela); Tel Aviv University (Taiber, Morozov)
"Because previous research indicates that vaccine compliance remains variable and inconsistent, successful inoculation against this disease will require widespread public educational campaigns regarding vaccine safety and efficacy."
With the global race to develop COVID-19 vaccines underway, there is a risk that concerns about the safety of such a vaccine could contribute to vaccine hesitancy and thereby threaten the uptake needed for herd immunity. To evaluate expected vaccination compliance rates among Israeli populations, a group of researchers distributed a multicentre questionnaire to medical staff and civilians across the country, inquiring whether they would agree to receive a SARS-CoV-2 vaccine once available.
The study is based on anonymous questionnaires distributed in April 2020, at the height of the first wave and at a time when Israel was under lockdown, to 1,941 participants. They included 1,112 members of the public (who are not healthcare workers), as well as 211 nurses and 338 doctors of both sexes from various medical specialisations, departments, and units, including coronavirus units, at hospitals throughout Israel.
Analysis revealed that the most significant positive predictor for acceptance of a potential COVID-19 vaccine is current influenza vaccination. Also, healthcare staff involved in the care of COVID-19-positive patients, as well as individuals considering themselves at risk of disease, were more likely to self-report acquiescence to COVID-19 vaccination if and when available.
In addition, there was a positive correlation between having become unemployed because of the coronavirus and willingness to get the vaccine - 92%, as compared to 72% among respondents who had been unemployed before the outbreak and 75% among employed respondents. This finding (that job insecurity due to the pandemic is a positive predictor for vaccine willingness) is in line with the assumption that the economic consequences of COVID-19-related restrictions would lead to an increase in compliance rates for potential future vaccines due to a desire to prevent lay-offs, high underemployment levels, and school closures.
The most dramatic finding was that only 61% of nurses would be willing to accept the vaccine. Among doctors, 78% said they would get vaccinated - only a bit more than in the general population (75%). This finding is surprising, per the researchers, because one might assume that the medical teams who are exposed to the patients and to the heavy burden of the disease would want to get vaccinated. The rate of acceptance for a COVID-19 vaccine among physicians and nurses overall is lower than their acceptance rates of seasonal influenza vaccination. Furthermore, only 55% of the nurses and 60% of the doctors said they would vaccinate their children against COVID-19, as compared to 70% of the general population.
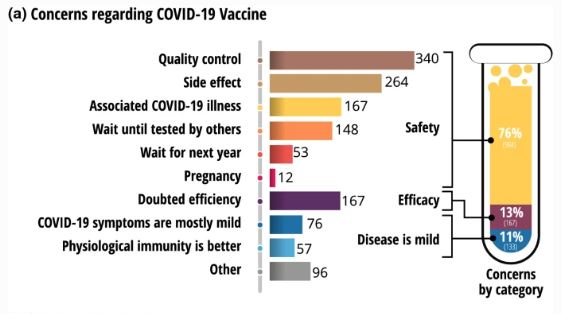
Seventy-six percent of the respondents - both in the general population and among healthcare workers - cited the issue of the safety of the vaccine as their most significant concern. Another 13% gave concern about side effects as a reason, and 11% said they saw the coronavirus as only a minor illness.
Reflecting on these findings, the researchers speculate that "emotional distress in the face of extensive media coverage of the rising numbers of casualties, overburdened health systems, and insufficient government responses to COVID-19 has perhaps fostered communal anxieties and distrust in preventative healthcare. These fears could also be contributing to wariness of the safety of a potential COVID-19 vaccine among the general public....[However,] the vast majority of the responders' concerns, among healthcare and non-healthcare workers alike, are due to the speed of [vaccine] development."
One worry is that lack of trust and willingness to get vaccinated among vaccine-hesitant healthcare workers could negatively impact the future vaccination compliance of members of the public who coincidentally engage with them on a professional or personal level. Thus, the researchers call for interventional educational campaigns targeted towards populations at risk of vaccine hesitancy in order to combat misinformation and avoid low inoculation rates.
In conclusion, this research demonstrates to policymakers, healthcare providers, and public health networks what advocacy needs to be done to encourage broad vaccination against COVID-19. In short, the scientific community "must act to educate, inform, and intervene to increase COVID-19 vaccine compliance rates in the entire population."
European Journal of Epidemiology https://doi.org/10.1007/s10654-020-00671-y; and "A Vaccine for Coronavirus? A Large Number of Israeli Doctors Will Refuse to Get It", by Ido Efrati, Haaretz, August 17 2020 - sent from Amiel A. Dror to The Communication Initiative on August 20 2020.
- Log in to post comments












































