Healthcare Provider Perspectives on the Uptake of the Human Papillomavirus Vaccine among Newcomers to Canada: A Qualitative Study
Ottawa Hospital Research Institute (Rubens-Augustson, L.A. Wilson, Murphy, K. Wilson); Lund University (Rubens-Augustson, Stafström); University of the Fraser Valley (Jardine); University of Ottawa (Pottie, Hui, K. Wilson); Bruyère Research Institute (Pottie)
"Creating language and culturally-appropriate information resources that promote knowledge and understanding of HPV vaccination will be fundamental..."
Newcomers, defined in Canada as foreign-born individuals who are immigrants, refugees, students, or undocumented migrants, face numerous barriers to human papillomavirus (HPV) vaccination. One study found that, among a female immigrant and refugee vaccine catch-up group, lack of knowledge was found to be the main barrier to vaccine series initiation, with most participants never receiving a healthcare provider recommendation. This is especially concerning given that immigrant and refugee women, who may not have attended cervical cancer screening in their country of origin and are less likely to attend pap smear screenings in Canada, are at a higher risk of developing cervical cancer. This study sought to understand, from the perspective of healthcare providers in Ottawa, Ontario, Canada, the barriers and facilitators to HPV vaccination and their recommendations to improve HPV vaccine uptake among newcomers.
A total of 10 healthcare providers were interviewed between March and April 2018. Five worked within the public health system, 4 were in primary care settings (2 family physicians and 2 nurse practitioners at community health centres), and 1 was a gynaecologist working in a hospital setting. Providers' perceptions of HPV vaccine uptake among newcomers were variable, with some providers feeling that coverage among newcomers was comparable to the general population, and others feeling that newcomers were more likely to reject the vaccine.
Categories of barriers to vaccination included:
- Access: Acknowledging that newcomers often find themselves in poor financial situations, providers were reluctant to recommend initiating a catch-up series, with some feeling uncomfortable recommending a vaccine that they could not provide for free. They also highlighted how difficulties accessing primary care and navigating a new health system in general could be a barrier to HPV vaccination among newcomers.
- Communication: Encountering newcomers who did not speak English or French severely limited providers' ability to explain the vaccine in detail and to ensure comprehension to enable the parent to make an informed vaccination decision. In addition, providers noted that health promotional resources were not at an appropriate literacy level for newcomers. Language barriers often manifested in issues with obtaining signed consent forms.
- Knowledge: All providers indicated that newcomer patients typically had very little, if any, previous knowledge about HPV, how it is transmitted, or the fact that there was a vaccine to protect against it.
- Culture: Providers discussed challenges with initiating discussions related to sexuality and sexual health, noting that this is often a taboo subject. Despite many newcomers being open to vaccination in general, some reported hesitancy to the HPV vaccine in particular, especially upon learning that HPV is sexually transmitted. Of newcomers who were hesitant to receive or rejected the vaccine, providers cited religious views as a factor that may impact vaccine uptake.
- Provider-related factors: Providers reported lacking the time or opportunity to engage with newcomer patients around the HPV vaccine, due in part to patients' tendency to seek care for acute issues rather than preventive care. In addition, a common practice among providers was to ensure that first and foremost, newcomers were up to date with the vaccines required to attend school.
Facilitators to HPV vaccine uptake included:
- Targeted health promotion: Providers working within the public health system recalled higher success in convincing newcomers to accept the vaccine in catch-up clinics, where they were able to have a face-to-face dialogue with parents and children.
- Efforts to understand the relevance of HPV vaccination: Providers mentioned that the recent decision to include boys in the school-based program would likely de-stigmatise the vaccine. Furthermore, some providers believed that lowering the age of vaccination against HPV and administering it at the same time as other vaccines would put it into the context of health, as opposed to sexuality.
- Trust in the healthcare system: Providers noted that newcomers displayed a great sense of openness to vaccination in general, in part because many of them have seen the health implications that can arise when people are not vaccinated in their country of origin; also, in their experience, newcomers were very trusting of the healthcare system and providers generally.
- Cultural sensitivity: Providers discussed the importance of culturally sensitive risk communication that emphasises cancer prevention to take the focus away from the vaccine's association with sexuality. They also highlighted providing access to female healthcare providers for female patients and having interpretation services readily available.
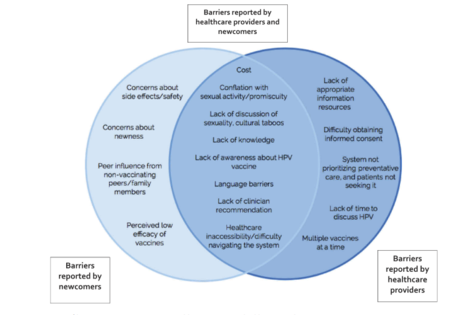
The results of the study also indicated that several perceived barriers were unique to newcomers or healthcare providers and did not appear across populations. In particular, barriers associated with vaccine hesitancy (e.g., concerns about side effects, efficacy, and the relative newness of the vaccine) were identified in a previous review as important obstacles for newcomers, but these issues were not mentioned by healthcare providers in the present study. By contrast, barriers that were uniquely identified by healthcare providers tended to refer to system-level barriers rather than the more individual-level barriers reported by newcomers. Two overarching recommendations were to publicly fund the HPV vaccine and to enhance language- and culturally-appropriate health promotion activities.
In sum, where immunisation programming for newcomers could be improved is at the structural and institutional levels, where information about HPV vaccination may not be conveyed in a way that meets the needs of newcomers. In addition to translated resources, one provider mentioned the importance of outreach to populations not currently accessing primary care. On that note, digital technology has been proposed as a potentially promising way of improving vaccine uptake and on-time vaccination by overcoming many of the barriers identified in this study, including the ability to track vaccination records when visiting multiple providers and provide reliable immunisation information. According to a needs assessment survey among newcomers in Ottawa, over three-quarters of participants indicated they would use mobile technology to track their vaccinations if it were available in their primary language. Given the near ubiquity of smartphones, leveraging digital technology may be a way forward in effectively disseminating vaccine information.
Looking ahead, the researchers welcome further research exploring informational desires and needs from the perspective of newcomers to inform strategies to promote equitable HPV vaccine coverage.
Human Vaccines & Immunotherapeutics https://doi.org/10.1080/21645515.2018.1539604
- Log in to post comments












































